MediCaring Communities: Introduction
Have you taken care of your mother or father as they lived out the last years of long lives? Or seen what happens to a friend’s parents, or someone else you knew and loved, who grew to be very old? Listen to how we talk about the experience. Mostly, we’ll experience travail, high costs, uncertainty, anxiety, frustration, and a generally difficult set of experiences. But sometimes things will go well—and the family caregivers and friends left behind will say, “Weren’t we lucky!” and go on to attribute the good luck to some specific happenstance. “My sister is a hospice nurse,” or “Our doctor was terrific,” or “Mom had the good sense to move into assisted housing and later to turn down most everything that the doctors suggested.” The reforms that this book presents—MediCaring Communities—aim to make it routine to get reliable and effective services, so that no one has to be lucky in order to have what they most need and want in old age. Let’s re-engineer the service delivery system to meet the needs we will have when old, at a cost that families and the society can afford!
Getting elder care right has never been more important. Just a few generations ago, people rarely survived into frail old age, and very few physicians thought that elders should be subjected to surgical operations or any other troublesome medical interventions. Most people still lived on farms, where there was usually room to take in a relative, and someone in the extended family was able to be nearby most of the time. For millions of Americans, their family members are now widely scattered, working full-time, or otherwise unavailable. Everything has changed, except for the love and concern of family members and friends. Most Americans now will live into advanced old age, usually with multiple chronic conditions, disabilities, and fragile health. For people alive at age 65, the average man can now expect 1.5 years and the average woman, 2.5 years, of needing someone’s help every day for “activities of daily living” like eating, toileting, moving about, and getting dressed.[3] But in most cases, our children can no longer take extended periods of time away from work to provide extensive direct supportive care, in part because they lack adequate retirement security for themselves. Many are also old enough to have some limitations themselves. A 95-year old mother may not be able to get much help from her two 70-something surviving children, both of whom are working part-time while dealing with their own arthritis and heart disease.
We forget that when Medicare started, 50 years ago, the average age at death was just 70 years old.[4] Now we get another decade, and that matters in many ways. The numbers are just starting to reshape the social order. Much more fundamental change is coming. Frail elders were rare in 1965 when Medicare started. Using age as a marker for frailty, the number of people 85 years old and older in the U.S. in 1960 was just under 1 million.[5] By 2000, we had 4.2 million.[6] By 2050, we’ll have 18 million.[7] People over 85 constitute the most rapidly growing part of the American population. Between 2010 and 2050, the under-15 population is projected to increase by only 17% while the number of people over 85 will increase by 231%.[8][9]
We have done very little to prepare for this aging population. The current “care system” developed around a different set of perspectives and demographic imperatives and it seriously fails to serve the needs and priorities of the frail elderly population now. Too many elders are hospitalized because we have no services standing ready to support them at home, or they have to move to nursing homes because we fail to make adapted and supported housing available. Elders routinely take inappropriate medications, suffer adverse events from errors in medications, are subjected to ill-advised tests, and undergo inappropriate treatments because the culture and the health care system fail to recognize that it is different to be living with serious progressive disability in old age than it is to be younger, with more resilience and more lifetime ahead. This mismanagement inflicts suffering on frail elderly people, uses up their savings, and wears out their family members.
Elders and their families deserve better—and we will deserve better in our own old age. But we will only achieve good care for frail elders if we learn how to stop the suffering, stop the waste, and stop the pretense that somehow just one more drug or medical breakthrough will make it all better and stave off death. In fact, what will make the lives of old people better is a thoughtfully arranged system that provides appropriate services at an affordable cost to them and society. Unlike some of the very difficult economic and environmental issues that face the country, a good plan is easy to find for the predictable rise in frail elders—that good plan is in this book! What we lack is only the energy and imagination to make it happen. That’s what this book hopes to change.
Signals of a willingness to undergo reform are beginning to appear. After decades of functioning as an insurance plan, Medicare has become an active participant in change, offering tests of new models and more aligned incentives at a remarkable rate. Academics and philanthropies now push for addressing problems with the social determinants of health and lament our society’s use of health care as an inadequate remedy for shortcomings in housing, food, jobs, and other constituents of good health. Financing of long-term care has come back to the policymaker agenda after a long hiatus.[10][11][12] The stage is set for serious and enduring reforms.[13]
This book proposes a thoroughly pragmatic plan—MediCaring Communities. The MediCaring reform process has six core components that fit together like the disparate elements of a machine that produces a good product only when all the parts work together. The following chapters will fill in the details and lay out a strategy for how to get from the here and now, with a care system that is indefensible and costly, to a future that bodes well for our ever-more diverse, multi-generational society.
The most dramatic changes from present practices are twofold. First, each frail elderly person has a unique set of hopes, priorities, strengths, personal resources, and medical conditions. Each person therefore needs a customized plan of services, not just the standard medical treatment for each malady. Second, support for each frail elderly person is anchored in his or her local community. Communities should play an important role in helping to plan and integrate the wide variety of services that elders need to stay out of crisis, and in co-managing improvement activities and funding priorities. At first, our proposed reforms may seem to be too difficult to engineer, but multiple strategies can work well, starting with the advantages some communities have because they have strong Programs of All-Inclusive Care for the Elderly, called “PACE.”
Core Components of a MediCaring Community
1. Frail elders identified in a geographic community
2. Longitudinal, comprehensive, elder-driven care plans
3. Medical care tailored to frail elders
4. Scope to include social and supportive services
5. Monitoring and improvement by a Community Board
6. Financing with savings from Medicare
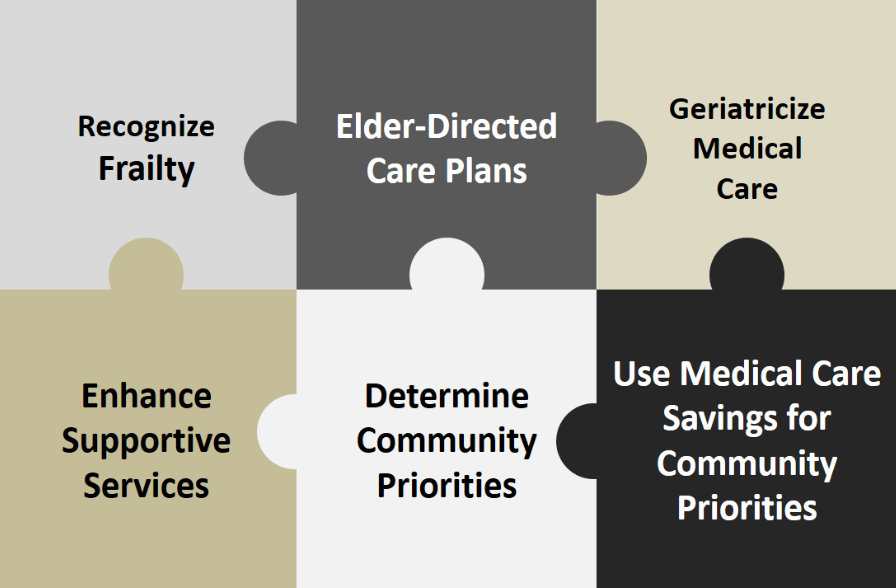
MediCaring Has Six Components
References
[3] (Favreault and Dey 2015)
[4] (United States Census Bureau 2003)
[5] (West, et al. 2014)
[6] (West, et al. 2014)
[7] (Ortman, Velkoff and Hogan 2014)
[8] (Pew Research Center 2014)
[9] (Administration on Aging, Administration for Community Living, Projected Future Growth of the Older Population 2005)
[10] (Favreault, Gleckman and Johnson 2015)
[11] (Hayes, et al. 2016)
[12] (LeadingAge 2016)
[13] (Lynn and Blair 2016)
MediCaring Communities: Getting What We Want and Need in Frail Old Age at an Affordable Cost
List Price $9.95 at Amazon.com
Published June, 2016
194 pages, 6″ x 9″ (15.24 x 22.86 cm)
ISBN-10: 1481266918

Click cover for Amazon.com
